Do Babies in Icu Get to Breast Feed
Abstruse
Objective:
Rates of breast milk feeding at hospital discharge are depression in premature infants due to the many associated challenges. Although there are many benefits associated with chest milk, the furnishings of direct breast-feeding in the neonatal intensive care unit (NICU) take not been identified. The purpose of this study was to investigate the human relationship between direct breast-feeding (babe sucking directly from the chest) and elapsing and success with breast milk feedings until discharge in premature infants.
Report Pattern:
This retrospective cohort was conducted on 66 very-low nascence weight infants whose mothers initiated chest milk feedings in the NICU. Chart review revealed documented type (chest milk with or without fortifiers or type of infant formula), volume and style (nasogastric tube, breast or canteen) of all gastric feeds for each day of NICU hospitalization. From this documentation, whether the mother initiated breast milk feedings, the number of times the mother put the infant to chest, the gestational historic period of the start direct breast-feeding, whether the offset oral feeding was at the breast, the elapsing of breast milk feedings and whether breast milk feedings connected until NICU belch were determined. Associations between breast-feeding participatory factors and breast milk feeding outcomes were investigated using linear and logistic regression.
Consequence:
Positive associations were found between breast milk feedings at discharge and mothers putting their infants directly to breast in the NICU (P=0.0005). The elapsing of breast milk feedings was associated with: mothers putting their infants directly to breast (P=0.0110), whether the first oral sucking feeding was at the breast (P=0.0108) and the gestational age of the showtime breast-feeding endeavor (P<0.0001).
Conclusion:
Breast milk feedings are encouraged in most NICU's, but directly chest-feeding is frequently overlooked as an of import area of enquiry in the tightly controlled surroundings of the NICU. This study demonstrates a link between straight breast-feeding behaviors in the NICU and success with provision of milk at discharge, as well equally how early participation can be an important factor in the breast-feeding procedure for mothers of NICU infants. More research on the effects of direct chest-feeding is warranted.
Introduction
Breast milk feedings in premature infants take been a focus of inquiry, and the multiple benefits of breast milk feedings for the premature babe take been established.ane Even so, breast milk feeding the premature babe and making the transition to sucking feedings at the breast (direct breast-feeding) come with meaning challenges.2
In the neonatal intensive care unit (NICU), there are many reasons why breast milk feedings fail to keep until hospital discharge. Frail, vulnerable, medically compromised infants often cannot eat past rima oris initially,3 and their mothers must regularly limited breast milk for gastric feedings, while maintaining their milk supply until direct breast-feedings are possible.4 Transitions from tube to oral feeding may not be possible until the infant is several months onetime. In add-on, the transition to total sucking feeds tin be dull, as poor oral motor skills and inefficient feeding are mutual among premature infants.v Initial direct breast-feeding attempts may consist of skin-to-skin contact or nuzzling at the breast while gavage feedings proceed. Every bit an infant becomes more mature, this can progress to brusk, inefficient periods of suckling at the breast with partial gavage supplementation. Finally, the babe is able to engage in longer, more efficient periods of oral sucking with or without boosted supplementation.
It is not uncommon for the mother of a premature infant to follow a rigorous pumping schedule for weeks or months without being able to put her infant directly to the chest. Declining milk supply is a common trouble associated with expressing breast milk and is cited as one of the biggest barriers to breast milk feeding the premature baby.2, 6 Although barriers to breast-feeding the high-risk baby take been studied and some treatments have been identified, there is a paucity of studies that accept investigated environmental factors that can influence success with breast milk feedings until NICU discharge. Although the benefits of participation in chest-feeding in the NICU tin be assumed, to date in that location take been no studies investigating the role of certain environmental factors or chest-feeding patterns in the NICU on breast-feeding success at belch. The objective of this study was to investigate ecology or participatory factors associated with the elapsing of chest milk feedings and success with breast milk feeding at NICU discharge.
Research questions
(i) Are there associations betwixt chest milk feedings at NICU discharge and:
-
The number of times an infant is put directly to breast in the NICU?
-
Whether an baby is always put straight to breast in the NICU?
-
Whether the outset oral sucking feeding is at the chest?
-
At what gestational historic period the infant is offset put directly to chest?
(2) Are there associations between the duration of breast milk feedings in the NICU and
-
The number of times an infant is put straight to chest in the NICU?
-
Whether an infant is e'er put straight to breast in the NICU?
-
Whether the outset oral sucking feeding is at the chest?
-
At what gestational historic period the infant is first put direct to chest?
(three) Are there associations between the number of direct breast-feeds in the NICU and
-
Whether the starting time oral sucking feed is at the breast?
-
At what gestational age the babe is start put directly to breast?
Methods
This study was a retrospective cohort, taking place in a 75-bed level 2 and 3 NICU in a midsized southern metropolis. The written report was canonical by the human subjects commission at the written report site. Informed consent was waived due to information drove being by a retrospective nautical chart review of information not deemed to be sensitive.
The written report sample consisted of subjects enrolled in a parent study investigating breast-feeding behaviors before and afterward a breast-feeding educational intervention. Subjects were sequent new admissions admitted during an 18-month menstruum. Parent study exclusion criteria were infants who weighed >1500 g at birth, infants who had a known built anomaly or other impairments that could contraindicate or impede oral feeding and infants who were admitted beyond the 7th 24-hour interval of life. For this written report, infants were also excluded if their mothers chose not to provide chest milk for the infant in the NICU or if the infant expired or was transferred to some other infirmary before discharge to home.
At the report site the blazon, book and manner of babe feeding are consistently documented by the nursing staff in each infant'southward medical chart following each infant feed. Retrospective chart review was conducted past the chief investigator and was checked for reliability by another researcher, with 100% reliability. From the daily recordings of type, volume and mode of infant feedings, the following data was collected: duration of breast milk feedings (the last day of life in the NICU the baby received any breast milk by breast, bottle or tube), whether breast milk feedings continued until discharge (whether or not the infant received whatever breast milk by breast, bottle or tube in the 24 h before the discharge), the gestational age at the first breast-feed (number of completed weeks of gestation when the babe first suckled direct from the chest), whether the first oral sucking feeding was at the breast, whether the mother ever attempted direct chest-feeding during the NICU stay and how many times the mother put the infant to breast during the NICU stay.
Associations between participation or environmental factors and success with chest milk feeding at discharge, duration of breast-milk feedings and the number of times chest-fed in the hospital were investigated using linear and logistic regression models with an α=0.05.
Results
The initial cohort consisted of 136 admissions of very-low birth weight infants admitted during the report dates. Of these, 52 were transferred to another NICU in the community or expired before discharge to home. Of the 84 infants discharged directly from the study site, 66 (79%) infants were provided chest milk subsequently nascency. Encounter Figure 1 for the patterns of breast milk feeding initiation and breast milk feeding at discharge among the 136 infants in the original cohort.
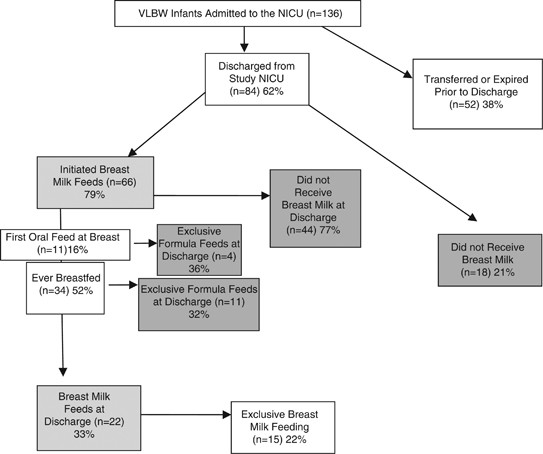
Patterns of breast milk feeding initiation and chest milk feeding at belch of the very-low birth weight sample.
Information from 66 mother–infant dyads who initiated chest milk feedings and were discharged from the study site were collected for this report. The range of gestational historic period at birth was 24 to 35 weeks, with the mean gestational historic period at birth of this sample being 28.i±2.7 weeks. The birth weight of the written report sample ranged from 550 to 1485 g with the mean birth weight being 1023±271 thou. Seventy-four percent (n=51) of the infants were part of a singleton pregnancy, with 26% (n=17) being a multiple birth. Forty-3 percent (n=28) of the sample was Caucasian, 47% (n=31) were African American and 9% (northward=6) were Hispanic. Thirty-i (n=20) percent of the sample were Medicaid eligible and 51% (due north=34) of mothers were married. The length of stay of the sample ranged from 10 to 108 days. The mean length of stay for the report sample was 66.4±27.four days.
Infants were beginning put to breast between 30 and 37 weeks gestation. The hateful gestational historic period at the first chest-feeding was 33.1±1.59 weeks. Only 16.iv% (n=11) of mothers who initiated chest milk feedings in the NICU had the first oral feeding at the breast. Among mothers who initiated breast milk feedings, fifty-two percent (n=34) breast-fed at least once during the NICU stay, with 48% (n=31) never breast-feeding in the hospital. Among mothers who initiated breast milk feeds in the NICU, the number of times the mother put her babe direct to breast while in the NICU was skewed toward 0. Withal, amidst mothers who put their infant to chest at least once during the NICU stay, the mean number of times breast-fed was thirteen.8±15.1 times. Of those who connected to provide breast milk until discharge, 100% had put their infants direct to breast at least once during the hospitalization.
The duration of breast milk feeds ranged from 12 to 108 days. The mean duration of breast milk feedings was 35.56±26.88 days. Of those who initiated breast milk feeds, 32.8% (n=22) continued to provide some breast milk at discharge (partial breast milk feeding), only only 22.4% (n=xv) provided sectional breast milk (100% of feeds were chest milk by chest or bottle) at discharge.
See Table 1 for factors associated with the outcome variables. Factors that were positively associated with breast milk feedings at discharge included number of times the infant was put directly to the chest in the infirmary (P=0.0005), equally well as, whether the infant was always put to breast (P<0.0001). Although the first oral sucking feeding being at the chest (P=0.0697) had a tendency toward significance, gestational age of the showtime directly chest-feed (P=0.4840) failed to demonstrate associations with breast milk feedings at discharge. Factors associated with the elapsing of breast milk feedings included the number of times the baby was put straight to breast (P=0.0110), whether the baby was ever directly breast-fed (P=0.0463), the first oral sucking feeding being at the breast (P=0.0108) and the gestational age at the first straight breast-feed (P<0.0001). Factors associated with the number of times directly chest-fed in the NICU included: whether the outset oral sucking feeding was at the chest (P<0.0001) and the gestational age of the get-go direct breast-feeding (P<0.0001).
Discussion
The fundamental findings of this study are that although maintaining breast milk feedings until NICU belch is a claiming for mothers, improved success is axiomatic amid mothers who have put their infants to breast during the hospital stay. In improver, having the first oral feeding be at the breast is associated with increased frequency of later chest-feeds, increased duration of breast milk feedings and trends toward increased success with breast milk feedings at hospital discharge. However, gestational age of the commencement direct breast-feeding was not associated with success with chest milk feedings at NICU discharge. Having the first oral feeding be at the breast and putting the premature infant to breast ofttimes in the NICU is important to enable breast milk feeding at NICU belch and beyond, even when early on chest-feeding is not possible.
One third of mothers, who intended to breast-feed and initiated the procedure of milk expression, succeeded with breast milk feedings until discharge. This is somewhat lower than previous studies that have reported rates of breast milk feedings at discharge between 36 and 61%.7, 8, 9, 10, 11 The exclusive breast milk feeding at discharge rate of 22.iv% was lower than previously reported rates of 31%.10 However, these previous studies have dissimilar operational definitions of breast-feeding at discharge (feeding directly from the breast versus having breast milk feeds from a canteen), in addition to have unlike cut-offs for gestational age at nascence and birth weight. In addition, many of the previous studies depict a rate of breast-feeding at discharge amongst all infants admitted to the NICU, whereas the current study reports chest milk feeds at discharge only amid those infants who had breast milk feedings initiated, which should yield a higher rate.
Diminished milk supply is i of the near significant barriers to breast milk feeding and chest-feeding the premature infant.2, 6 Ameliorate understanding why and how milk supply diminishes amid those who initiate breast milk feedings and determining constructive interventions to promote improved chest milk feedings and breast-feeding in the premature infant is of keen importance. Owing to its relationship with breast milk feedings at discharge, this research supports early on and frequent participation in straight chest-feeding in the NICU. In that location are physiological and psychological reasons as to why participatory factors could exist associated with whether a mother succeeds with providing breast milk through until NICU discharge.
A chest pump serves equally a necessary exchange for direct breast-feeding in the early on preterm baby, but the mechanism of milk expression differs from the infant suckling directly from the breast. An infant's broad open mouth position on the areola compresses milk out of the lactiferous sinuses and the rhythmic suckling response at the breast stimulates pulsatile release of oxytocin resulting in the milk ejection response. Milk flows through the ducts, followed past stimulation of more than milk production by the secretory cells. During baby sucking at the breast, a surge in prolactin also contributes to milk production. Manual milk expression fails to provide the compression that fully empties the sinuses, elicitation of the milk ejection response tin can be more difficult and in that location tin can exist inadequate prolactin release.12 Subsequently, milk production tin be impeded in mothers who cannot engage in direct breast-feeding with their medically delicate, premature infants.
At that place can also exist psychological benefits associated with direct breast-feeding. Oxytocin release has been identified earlier infant suckling at the chest, as a result of the maternal response to infant crying or in training for infant feeding.13 This would suggest that in that location is a circuitous machinery of mother–infant responses associated with the process of direct chest-feeding that possibly has non been fully realized. In addition, stress has been shown to be associated with difficulty in achieving oxytocin release and the milk ejection response,14 which tin interfere with adequate milk expression in mothers experiencing the stress of having an infant in the NICU. Although stress can interfere with oxytocin release, the release of oxytocin associated with the babe suckling directly from the chest can mediate stress.15, xvi Finally, the NICU is an environs where parents have reported feeling like an outsider and not being able to parent their infant.17, xviii, 19 Through participation in chest-feeding, mothers are given an active and meaningful function in the NICU, which tin build confidence and enable parents to handle and intendance for their infant.
The gestational age at which the infant is first put to chest and whether a mother puts her infant directly to breast for the showtime oral suckling feed tin can exist multifactorial. By agreement a trend toward improved breast milk feedings at discharge in infants who had the get-go oral feeding at the chest, health care professionals tin can better understand the importance of enabling the commencement oral suckling feeding to exist at the breast. Although the gestational age that the infant is first put to breast is associated with the number of times the infant is breast-fed in the NICU, at that place was non an association with breast milk feedings at discharge. This can provide some hope for those infants who cannot be breast-fed early, equally inability to engage in early breast-feeding does not brand later breast milk feeds unobtainable. All the same, by fostering straight breast-feeding as early on every bit possible and enabling the start oral feed to be at the breast, the number of times an infant is directly chest-fed can be fostered and potentially improve success with chest milk feedings until discharge.
This study demonstrates a link between direct breast-feeding behaviors in the hospital and the power to maintain breast milk feedings until hospital discharge. All mothers who initiated breast milk feedings but did non put their infants to breast in the NICU were no longer providing breast milk for their infants at NICU belch. The feel of ever breast-feeding the infant in the NICU, too as the frequency of direct chest-feeds, can accept positive effects on enabling the breast-feeding procedure until discharge and beyond. This supports other research that has identified predictive factors associated with breast-feeding in the NICU and described trends in improved duration of chest milk feeds among those who have infants directly suckling from the breast.20
Often the importance of direct suckling from the chest is overlooked in the NICU equally mothers express their milk, and it is given through a gastric tube or bottle. Withal, the duration of breast milk feedings in premature infants is low, indicating that mothers often cannot continue to efficiently limited milk indefinitely. The average duration of breast milk feedings was 36 days. Many very-depression birth weight infants volition necessitate gavage supplementation for longer than 36 days, however, this does not foreclose direct breast-feeding. Participation in the direct chest-feeding procedure during the transition from gavage to oral feedings, while continuing manual milk expression and supplementation, could be a disquisitional intervention that could foster success with breast milk feedings until discharge.
At that place were limitations to the current written report. This written report relied on when the babe was given breast milk, which did not necessarily define when the mother expressed milk and for how long she maintained her milk supply. Mothers who had backlog, frozen milk from early on milk expression could have had documented breast milk at discharge, even in the absenteeism of this factor. The pocket-sized sample size prevented investigating the effect of straight breast-feeding in specific demographic groups of mother–infant dyads. Another important limitation is related to variations in clinical condition and medical status, which can affect breast-feeding outcome. These variations in clinical condition may well have affected the success or failure of direct breast-feeding and take obfuscated the actual result of direct chest-feeding on subsequent success of breast milk feedings. Finally, although an association is evident, this study does not allow an interpretation of whether it is the participation itself that promotes success until belch or if information technology is that mothers who are more likely to succeed participate in breast-feeding in the NICU.
Conclusion
The findings of this study demonstrate a link between participation in straight breast-feeding in the NICU and duration of breast milk feedings, besides equally success with continued breast milk feedings until NICU discharge. The gestational historic period of the first direct breast-feeding and the outset oral suckling feeding being at the breast are associated with the elapsing of breast milk feedings, as well every bit with the number of times the infant is directly breast-fed in the NICU. Based on positive associations with breast milk feeding outcome, direct breast-feeding in the NICU could be a valuable breast-feeding intervention. Future studies are warranted to further investigate factors that tin positively influence breast milk feedings in the NICU and to investigate the effects of direct breast-feeding on baby and mother.
References
-
Gartner LM, Morton J, Lawrence RA, Naylor AJ, O'Hare D, Schanler RJ et al. Breastfeeding and the use of man milk. Pediatrics 2005; 115 (2): 496–506.
-
Callen J, Pinelli J . A review of the literature examining the benefits and challenges, incidence and duration, and barriers to breastfeeding in preterm infants. Adv Neonatal Care 2005; v (2): 72–88; quiz 89–92.
-
Hill PD, Andersen JL, Ledbetter RJ . Delayed initiation of breast-feeding the preterm infant. J Perinat Neonatal Nurs 1995; ix (2): x–20.
-
de Azevedo M, Mendes EN . Maintenance of lactation: a claiming for hospitalized premature infant'southward mothers. Rev Gaucha Enferm 2008; 29 (one): 68–75.
-
McGrath JM, Braescu AV . State of the science: feeding readiness in the preterm infant. J Perinat Neonatal Nurs 2004; xviii (iv): 353–368; quiz 369–lxx.
-
Kavanaugh K, Mead Fifty, Meier P, Mangurten HH . Getting enough: mothers' concerns about breastfeeding a preterm babe after discharge. J Obstet Gynecol Neonatal Nurs 1995; 24 (1): 23–32.
-
Pineda RG, Foss J, Richards L, Pane CA . Breastfeeding changes for VLBW infants in the NICU following staff education. Neonatal Netw 2009; 28 (5): 311–319.
-
Yip Eastward, Lee J, Sheehy Y . Breast-feeding in neonatal intensive intendance. J Paediatr Child Health 1996; 32 (four): 296–298.
-
Powers NG, Bloom B, Peabody J, Clark R . Site of intendance influences breastmilk feedings at NICU discharge. J Perinatol 2003; 23 (1): 10–13.
-
Davanzo R, Ronfani L, Brovedani P, Demarini S, Breastfeeding in Neonatal Intensive Intendance Unit of measurement Report Group. Breast feeding very-depression-birthweight infants at discharge: a multicentre study using WHO definitions. Paediatr Perinat Epidemiol 2009; 23 (6): 591–596.
-
Lee HC, Gould JB . Factors influencing breast milk versus formula feeding at discharge for very low nascency weight infants in California. J Pediatr 2009; 155 (5): 657–662 e1–2.
-
Yokoyama Y, Ueda T, Irahara Chiliad, Aono T . Releases of oxytocin and prolactin during breast massage and suckling in puerperal women. Eur J Obstet Gynecol Reprod Biol 1994; 53 (1): 17–20.
-
McNeilly AS, Robinson IC, Houston MJ, Howie Prisoner of war . Release of oxytocin and prolactin in response to suckling. Br Med J (Clin Res Ed) 1983; 286 (6361): 257–259.
-
Ueda T, Yokoyama Y, Irahara M, Aono T . Influence of psychological stress on suckling-induced pulsatile oxytocin release. Obstet Gynecol 1994; 84 (two): 259–262.
-
Heinrichs M, Meinlschmidt G, Neumann I, Wagner S, Kirschbaum C, Ehlert U et al. Effects of suckling on hypothalamic–pituitary–adrenal axis responses to psychosocial stress in postpartum lactating women. J Clin Endocrinol Metab 2001; 86 (10): 4798–4804.
-
Heinrichs Thousand, Neumann I, Ehlert U . Lactation and stress: protective effects of chest-feeding in humans. Stress 2002; v (3): 195–203.
-
Lupton D, Fenwick J . 'They've forgotten that I'thousand the mum': amalgam and practising motherhood in special care nurseries. Soc Sci Med 2001; 53 (viii): 1011–1021.
-
Aagaard H, Hall EO . Mothers' experiences of having a preterm babe in the neonatal care unit: a meta-synthesis. J Pediatr Nurs 2008; 23 (three): e26–e36.
-
Wigert H, Johansson R, Berg M, Hellström AL . Mothers' experiences of having their newborn child in a neonatal intensive care unit of measurement. Scand J Caring Sci 2006; 20 (one): 35–41.
-
Smith MM, Durkin M, Hinton VJ, Bellinger D, Kuhn L . Initiation of breastfeeding among mothers of very low birth weight infants. Pediatrics 2003; 111 (six Part ane): 1337–1342.
Author information
Affiliations
Corresponding author
Ideals declarations
Competing interests
The author declares no conflict of interest.
Rights and permissions
About this commodity
Cite this article
Pineda, R. Direct breast-feeding in the neonatal intensive care unit of measurement: is it important?. J Perinatol 31, 540–545 (2011). https://doi.org/ten.1038/jp.2010.205
-
Received:
-
Revised:
-
Accepted:
-
Published:
-
Issue Date:
-
DOI : https://doi.org/10.1038/jp.2010.205
Keywords
- NICU
- breast-feeding
- chest milk feedings
- participation
- intervention
- premature infants
Further reading
Source: https://www.nature.com/articles/jp2010205
Post a Comment for "Do Babies in Icu Get to Breast Feed"